Glaucoma Consults Round-up: Pt 2. Sep 28 - Oct 2, 2009 In-depth case discussions.
/Friday October 2, 2009 & October 29, 2012
Another article recovered from the migration and available to all to enjoy.
Case 9:
robschertzer #glaucoma #consult 41 yo WM, from optom ?NTG w/ sup rim VF def OU; on O/E v periph TI defects, flat irides burned out PDS?
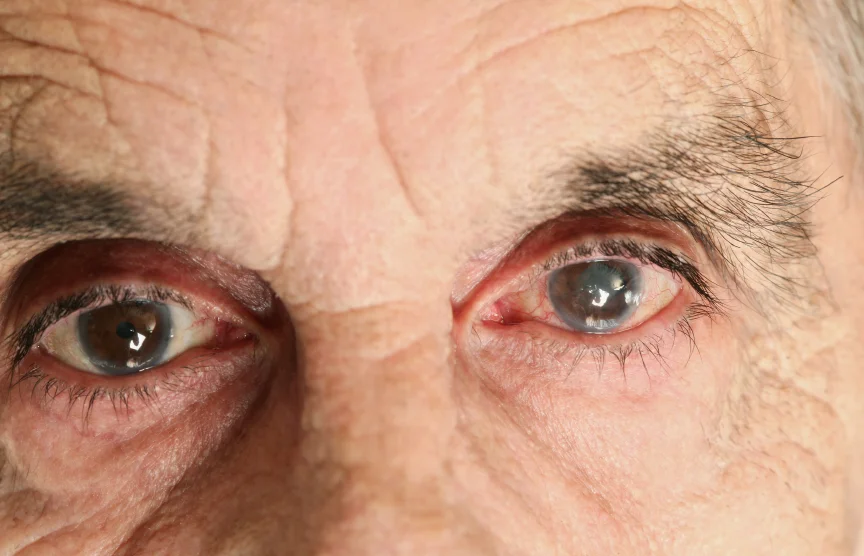
These patients was referred by his optometrist as a glaucoma suspect on the basis of increased optic nerve cupping and a possible early visual field defect. There was no positive family history of glaucoma. The patient had a mild hyperopic astigmatism with best corrected visual acuity of 6/7.5 OU. IOP readings were 14 OU @0915hrs, corneas of normal thickness at 544 and 551 ums. The iris contour was flat with some small and very peripheral transillumination defects, mostly inferiorly. There was also mild to moderate increased pigmentation of the angle structures in a patchy distribution. The Visual Field is as depicted below.
The baseline HRT is depicted below. Of note here is a rim area at the low end of the normal range.
This case really illustrates how things are not always clear cut on initial assessment of patients suspected of having glaucoma for several reasons from findings in the clinical examination to the use of ancillary test results to draw conclusions.
This patient was initially evaluated by one of our Ophthalmology Residents rotating through glaucoma, and he was wondering if this patient has pigmentary glaucoma. Although there were some traces of transillumination defects, one of the findings seen in pigment dispersion syndrome & pigmentary glaucoma, other features of the disorder were absent. In fact, the nature of the transillumination defects were not quite right and are shown properly in the link to the pigmentary glaucoma article. Oftentimes, patients with very lightly pigmented irides can show transillumination defects at the extreme periphery of the iris just form their lack of iris pigment. These should not be confused with the slit-like defects in pigment dispersion syndrome that have a gap of normal iris between the peripheral end of the defect and the peripheral iris. This patient also did not have the characteristic Krukenberg Spindle on the corneal endothelium or the pathognomonic Scheie's Line of pigmentation behind the lens where the vitreous humor comes into contact with the lens.
With regard to the use of ancillary tests for glaucoma, it should always be remembered that tests such as the Visual Field and HRT nerve scan are meant to complement the clinical picture and are not, on their own, diagnostic of anything. For this patient, the peripheral nature of the Visual Field defect can be just the upper eyelids interfering or may represent true glaucoma damage. The HRT nerve scan shows that the area of the neuroretinal rim is at the low end of the normal range but this can just be the way the patient was born.
2Oct2009 Case 9 VF OS
2Oct2009 Case 9 VF OD
In summary, this patient may end up having early glaucoma but may just as likely not have glaucoma at all. We really need to follow the patient over time to see if we see loss of neuroretinal rim tissue or changes on the visual field over time. In addition, the eye pressures may change over the follow-up period and could even be fluctuating over the course of each day.
Case 10:
robschertzer #glaucoma #consult 52 yo Asian M, v high myope, v tilted discs, N CCT: no glaucoma but follow.
A picture is worth a thousand words here; OK, actually an HRT scan but close enough to a picture for the purposes of discussion.
2Oct2009 Case 10 HRT OS
Case 11:
robschertzer #glaucoma #consult 61 yo Asian M Tx'd w/ Lumigan for NTG, also high BP, thin inf optic N rims; taking over care.
This patient with Normal Tension Glaucoma (NTG) was referred by another ophthalmologist to help take over his care. Despite IOP readings of 10 mmHg in both eyes, there was concern that his glaucoma could still be progressing in the right eye. There was more 'cupping' of the right optic nerve than the left with the neuroretinal rims NOT notched right out to the rim in either eye. The most recent Visual Field provided by the referring doc was from April 2009.
2Oct2009 Case 11 VF OD
This patient was referred with insufficient information to draw any conclusions at this time. One VF from 2004 then one from April 2009 is not sufficient to tell if a patient is stable right now. Although there is a change, this may have all occurred as much as 5 years ago and may have been stable ever since. We can at least repeat the VF now to see how it compares to the one from this past April, but will likely need more data than that to confirm progression. In fact, this VF was essentially normal in the eye of concern:
Case 12:
robschertzer #glaucoma #consult 87 yo WF, max meds, pseudophakic, prior massive chroidal heme OD during Trab; opt SLT only even if low success odds.
This patient was referred from out of town with a cataract and COAG with pressures ranging from 12 to the low 20s taking Travatan, Combigan, and Azopt. The challenge here is that she was blinded in her right eye when cataract surgery resulted in a choroidal hemmorhage. She has noted a decline in vision but it is not certain how much of this is progression of her cataract vs glaucoma. Nonetheless, if she were to hemmorhage in her only eye on any attempted surgical intervention, she would be much worse off. Hence the decision to try a Selective Laser Trabeculoplasty (SLT) even though the odds of this having a big effect on lowering the IOP when she is already on four glaucoma medication (Combigan combines Alphagan with Timolol) is not very good. At least we are trying to do something to minimize the chance of her glaucoma getting worse in her lifetime.
Case 13:
robschertzer #glaucoma #consult 66 yo WF, NTG on Lumigan w/IOP 18 & 17, N CCT, no meds making diff, VF defect central OU; no proof progression yet.
This patient poses another common management dilemma, again centred around documentation to confirm whether there is progressive glaucomatous damage. This patient has normal tension glaucoma and, as can often be seen in this type of glaucoma, the damage is close to the centre of her vision (close to fixation.) However, just because the visual field defect is near the centre of a patient's vision does not mean that they are at any higher risk of their glaucoma progressing. Dr Drance discussed this with me in one of our Talking About Glaucoma podcasts on Normal Tension Glaucoma.
2Oct2009 Case 13 VF OD
After discussing with the patient that we did not have enough information to tell if she is at risk of her visual field progressing, I called the referring ophthalmologist to discuss a plan. He will repeat the Visual Field test soon and keep repeating every 4 months to look for any hints of progression. Again, a key teaching point here is that just because the visual field defect is near the centre of this patient's vision, it may very well have been this way for many years and could actually be stable. Why expose the patient to the added complications of surgery if not necessary.
Case 14:
robschertzer #glaucoma #consult 82 yo WM, PXF & pseudophakic, IOP 31 on max meds; clearly needs Trabeculectomy with MMC
This is one of the most foregone conclusions in that the patient has Pseudoexfoliaton Glaucoma, notorious for suddenly tipping out of control, and the fact that they were referred by another glaucoma specialist who no longer performs glaucoma surgery. Their IOP was just 9 OD but 31 OS taking Pilocarpine 4%, DuoTrav and Azopt. They have previously had a Selective Laser Trabeculoplasty in the left eye and cataract surgery in both eyes.