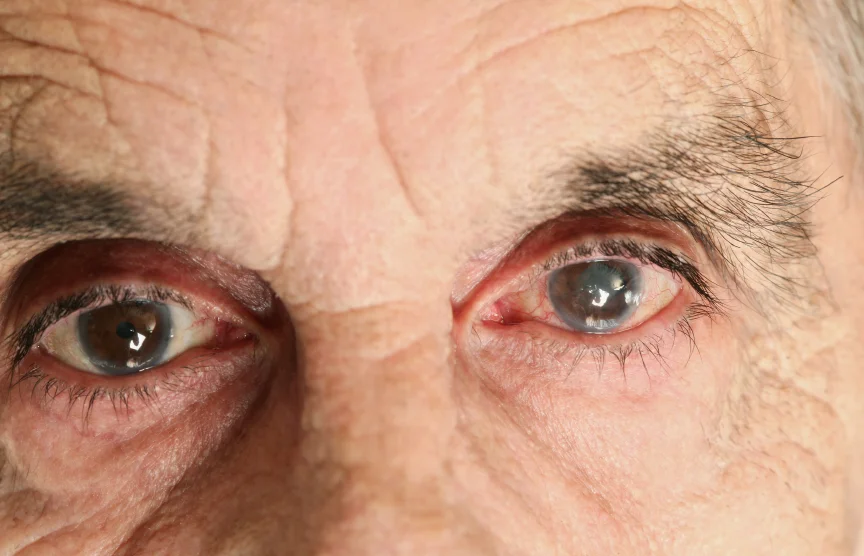
Retained lens fragment and subluxed IOL chafing induced post-op glaucoma
/Subluxed IOL and TI defect - photo by Raymond Mok
A 74 year old female presented after recently having cataract surgery elsewhere two weeks earlier. She had previous open angle glaucoma stable taking just Azopt OU BID. The capsular bag had been broken at the time of the cataract surgery, there were retained lens fragments and the eye pressure was rising. Travatan qHS and Combigan TID had already been added (yes, TID), and she was also on Ketorolac, PredForte and Vigamox each TID in the operated eye. This patient is also on Coumadin. In addition, the surgeon had brought her back to the operating room 8 days later to remove the retained cortical fragments and has performed several in-office paracenteses as the pressure was up to 51 mmHg. After two weeks of this, the patient came to see me for help.
Cortical fragments at 6:00 - photo by Raymond Mok
On examination her vision was 20/150 in the operated eye, improving to 20/70 with pinhole. The cornea showed 2+ edema, there were lens fragments in the central AC, in the angle and in the bag. The IOL was subluxed and a few clock hours of her nasal iris had been chaffed away from where the tilted edge of the IOL had been rubbing. Her IOP was down to 30 mmHg. I performed urgent surgery the following day not knowing if I could salvage the lens implant or if an AC lens would be needed, combined with a trabeculectomy with Mitomycin-C.
As per a combined phaco/trab surgery, I began with the opening steps of a trabeculectomy from above then moved temporally before completing the trabeculectomy scleral flap. I used provisc and viscoat to help keep the IOL from sinking and to protect the cornea. After rotating the optic and one of the two haptics into the anterior chamber, I used IOL micro-grasping forceps to hold the lens while performing automated irrigation and aspiration of the retained lens fragments. Under viscoelastic, I was able to reposition the haptics in the sulcus and capture the optic in the bag. Verifying that the lens was stable, I completed the trabeculectomy and called it a day.