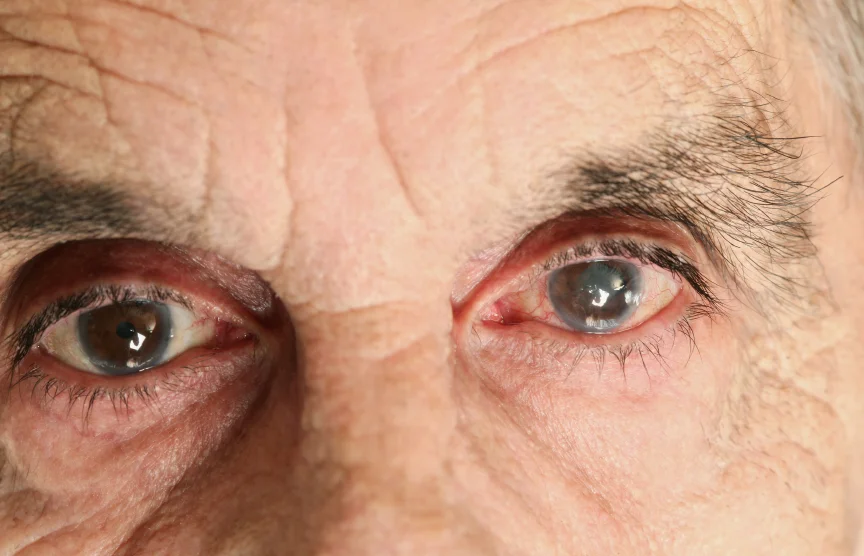
Glaucoma horror story of the week 13 yo girl presenting with IOP = 50 and advanced damage; how can this happen?
/Tuesday November 10, 2009
robschertzer #Glaucoma #consult 13 yo Middle Eastern F, IOP 50 & 48, CCT 529 & 531, near total cupping, spont venous pulsations, YIKES!!
This is the horror story glaucoma case of the week. It leaves us to wonder how long this has been going on? Could this have been prevented? What are the best treatment options? What is the prognosis?
10Nove2009 Case 1 HRT OS
10Nov2009 Case 1 HRT OD
This 13 yo middle eastern girl was referred to me due to increased optic nerve cupping, high intraocular pressure and abnormal visual field by an optometrist. She is an 8D myope who has been seen annually by an optometrist, albeit a different one each visit, from the same office. She is noted to have a visual acuity of 6/7.5 OD and 6/9 OS with her current spectacle correction, IOP readings of 50 OD and 48 OS by Goldmann applanation tonometry at 1500hrs, and slightly thin corneas measuring 529 and 531 ums. She was understandably quite upset having been referred to see me urgently which made for some trouble completing the gonioscopy so I could not get a proper look at her angles to confirm whether there was a congenital angle appearance. Her anterior chamber was deep. As can also be noted on the HRT scans, she has quite damaged appearing optic nerves with thinning of all rims.
10Nov2009 Case 1 VF OS
10Nov2009 Case 1 VF OD
Visual Field testing was performed as noted here as well. Given the other strong clinical evidence of glaucoma damage, even though the VF was quite unreliable in terms of false positive and false negative responses which can make one ignore the findings without repeating them, much of the missed points must represent damage.
This patient has been followed annually for five years yet has massive glaucomatous damage. How could this have been missed since we would never want to see this happen to anyone else and need to know how we can prevent missing glaucoma in a child. We tend to think of glaucoma as something that you either come out of the womb with, or that you get sometime after 40 years of age. If I saw these findings in an adult, I would probably jump to the conclusion that this patient has had glaucoma for many years to end up with this much damage. Nobody really knows how long the permanent damage takes to develop in glaucoma, and certainly the level of the pressure as well as the duration of this rise must contribute along with the vascular state. But do these same rules apply in children? There is more elasticity in children so perhaps some of her damage is actually reversible. I have seen some reversal of cupping on the rare occasion in which I've treated paediatric patients with glaucoma. I only cover childhood glaucoma on rare occasions in which the paediatric ophthalmologist who handles all the childhood glaucoma is out of the country for a prolonged period of time. Congenital glaucoma tends to require surgery as an early intervention which I cannot perform at my hospital as the patient is under 16 years of age.
That being said, I did refer this patient on to see Dr Lyons. He was able to complete the gonioscopy portion of the examination to confirm the anterior insertion of the angle structures consistent with congenital glaucoma. In addition, with his training as a paediatric ophthalmologist, he performed a more complete genetic history and examination to reveal that this patient had her teeth capped as they were pointy and took the liberty of examining her younger sister who showed some similar findings to a lesser degree and lacked the elevated eye pressures. Dr Lyons did start this patient on medical therapy to which she did show some response when followed up the following day. He will likely bring the patient to the operating room in the near future for angle surgery.
This patient has a congenital glaucoma and likely her little sister is effected as well. I will be seeing her parents to see if they are showing any glaucoma findings as well. Given the greater elasticity of tissues in children, it is hoped that the damage will be somewhat reversible and the parents are grateful to at least know that we can intervene to stop things from progressing significantly. It is quite possible that this little girl did not have glaucomatous damage one year prior when last seen by an optometrist. I am cautiously optimistic.
I am also wondering if anyone has had a similar patient and has some further thoughts on their care. Please add your comments below.