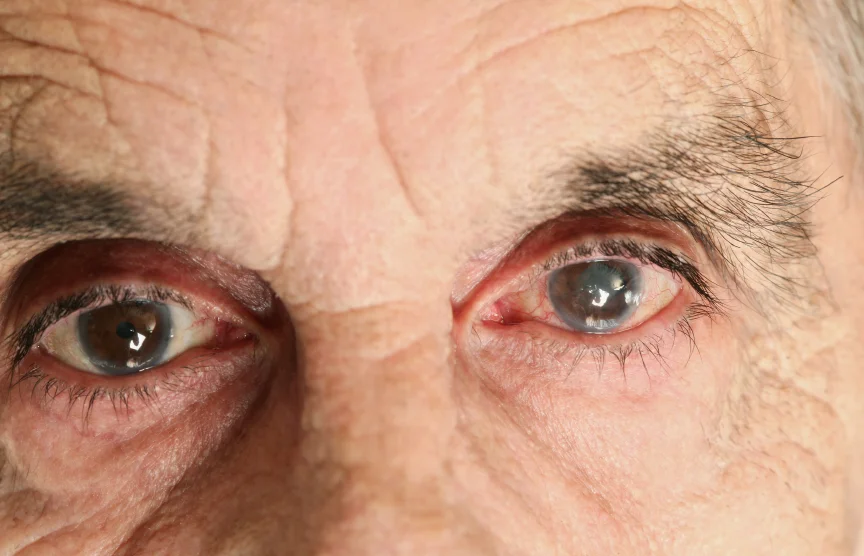
Glaucoma surgery round-up: The art of teaching glaucoma surgery and follow-up care?
/A recap of this past week's tweets of 3 glaucoma surgeries. A relatively light surgical week with only three patients but always something to learn from everyone. This week I talk about how I teach glaucoma surgery. This article contains additional information not found in the original 140 character postings including the findings at the 1 day and 1 week post-op visits. Please add your comments so that we can extend these teachable moments over time.
Tuesday October 6, 2009
robschertzer #glaucoma #surgery 62 yo E Indian F, COAG phakic progressing w/ IOP 14-20 max tolerated meds- Trab MMC OD; OS to follow future.
It was non-compliance to medical therapy that led to this patient with Chronic Open Angle Glaucoma ending up in the operating room for a trabeculectomy. They were showing progression on their visual field and HRT nerve scan, therefore changes in both function and form of the optic nerve.
The surgery was actually without complications but a point worth discussing is how we go about teaching glaucoma surgery to ophthalmologists-in-training (residents.) At our institute, the UBC Eye Care Centre, I am actively involved with training residents as well as glaucoma fellows (ophthalmologists subspecializing in glaucoma.) There is only so much that can be learned by reading books and practicing on cadaver or animal eyes as neither of these are close enough to the real thing. Therefore, residents do need to operate on real living patients in a safe environment, under the watchful eyes of experienced surgeons so that they can operate on their own in the future. I am honoured to help train residents and fellows in performing glaucoma surgery and do so in a graduated approach.
The approach I use in the hands-on teaching of glaucoma surgery involves gradually performing different parts of different procedures and allowing them to proceed to other steps once other steps are mastered. The first test is just seeing how attentive the trainee is as an assistant. If they don't seem to know what is going on, they don't move on to the next step - that of actually doing anything! Their ability to cut stitches that I tie is the next hurdle; if they can't quite tell where the suture is accurately, they will be stuck assisting for a long time. When they have gained my confidence, I start allowing them to perform a single step of the surgery, with me assisting them, usually starting with the last step which is closing of the conjunctiva (the outer most layer of the eye.) They will then slowly work backwards doing more of the steps in future surgery cases and allowed to progress at their own level so as to make sure they are learning and above all causing no harm. Some trainees, by the end of their weekly apprenticeship over a two month period are doing complete glaucoma surgery cases whereas others may still just be doing some steps but not full cases. In the end, they all learn to the best of their abilities and patients are safe.
The first post-operative visit was later the same day when the patient called because of pain at which time the IOP was 54 with a fairly flat bleb. Gentle compression of the eye from below brought the pressure down to just 7 mmHg. The patient was maintained on the usual protocol of prednisolone acetate drops every 2 hours while awake and Vigamox antibiotic drops 4 times daily with an appointment to return the following week.
The patient's IOP was 40 on the first post-operative day and required a repeat eye massage. She was instructed on how to massage here own eye several times per day leading up to her 1 week visit but she didn't bother as she was no longer in pain after the first day. Despite the lack of pain, her IOP was 42 at the one week visit and I needed to compress on her eye again from the 6:00 position through closed eyelids with her looking upward. The pressure did go down to 4 mmHg with the bleb raising up nicely.
Much of the time, there is more involved in the post-operative period in caring for patients with glaucoma filtration surgery than the surgery itself. In fact, some say that anyone can 'put a hole in the eye,' but without proper post-operative care, the surgery can fail.
robschertzer #glaucoma #surgery 72 yo WM PXF phakic, DuoTrav & Azopt max tolerated pre-op; performed Trab MMC
This patient was referred by a medical glaucoma specialist with 'severe pseudoexfoliative glaucoma.' Patient was first seen by the referring ophthalmologist in May 2008 with advanced damage and every time a medication was added, it would drop the eye pressure to the mid teens only to bounce back into the low 20s soon afterwards. The defect in his visual field was approaching the centre of his vision ('threatening fixation.')
Again the surgery was without complications but the pressure was 33 on the first post-operative day until the eye was massaged down to an IOP of 16. As with the other patient, the patient was 40 with a fairly flat bleb at the first week but compressed down to just 3 with the bleb raising nicely.
There is the option when performing a trabeculectomy of using the Optonol ExPress mini-shunt. Although there has yet to be conclusive evidence of a longterm advantage of using this shunt, there is evidence that the early post-operative period is more stable, with less of these big swings in eye pressure. Unfortunately, this little metal stent costs $950 and is not covered by our hospital so the patient has to be out of pocket for this implant at this time. (This may be different in your area.)
robschertzer #glaucoma #surgery 64 yo WF prog COAG phakic IOP 12-18 Alphagan, Xalatan, Cosopt: Trab MMC performed. More details 2 follow w/ wk roundup.
This patient was referred from a remote area with a documented history of progressing over the past 4-5 years despite her current therapy. Surgery was uneventful as per the other two patients. Unfortunately, all of their follow-up care is being done back in the remote area by the referring ophthalmologist. From the prior two cases today, you can see why I would prefer seeing my patients back for ALL of their post-operative visits. Unlike cataract surgery, glaucoma has a much more unpredictable post-operative course and requires frequent follow-up care and interventions to get good longterm outcomes.