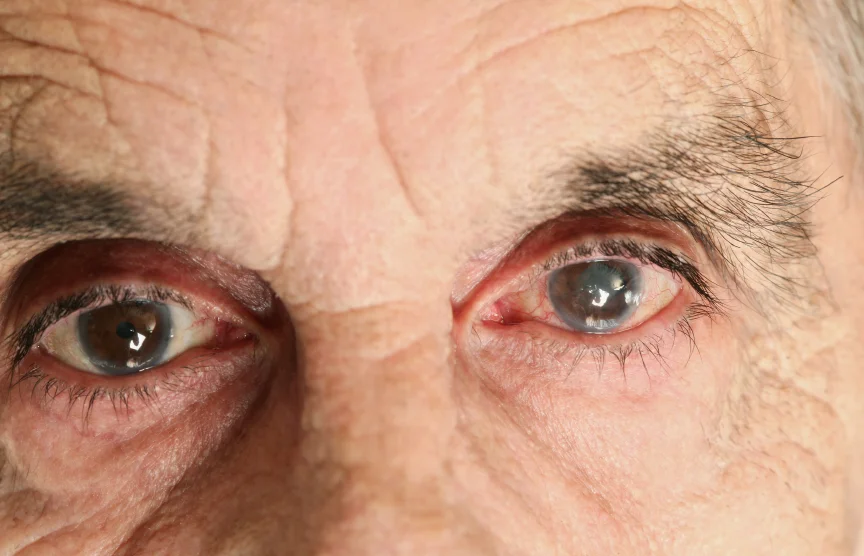
This past week in Glaucoma Surgery Sept 21-25, 2009
/A recap of this past week's tweets of 9 glaucoma surgeries and 4 cataract surgeries in my glaucoma patients. This article contains additional information not found in the original 140 character postings. Please add your comments so that we can extend these teachable moments over time.
21Sep2009
Case 1:
robschertzer #glaucoma #surgery 21Sep2009, 49 yo WF, raised epsicleral venous pressure, failed medTx; Trab MMC minimal bleeding, phew!
Despite a complete neurological investigation, no cause had been found to date to explain the raised episcleral venous pressure in this patient. Nonetheless, despite medical therapy, she has been showing progressive glaucomatous damage to her right optic nerve requiring surgical intervention. Although she has enlarged and slightly tortuous vessels on the surface of her eye, these were not the result of inflammation and were therefore not friable/leaky. Although there was a bit of extra bleeding, it was far less than one would expect with the presence of extra vessels on the surface of the eye.
On the first post-operative day, her IOP was down to 3 with visual acuity of 6/30 that improved by pinhole to 6/18. Her pre-operative visual acuity was 6/6 with IOP of 24. As her anterior chamber was only 1-2 corneal thicknesses deep centrally, I started her on Atropine 1% drops TID in order to pull back the ciliary body to deepen the chamber.
Case 2:
robschertzer #glaucoma #surgery 21Sep2009 73 yo hispanic F, COAG w/dense cataract; combined trabMMC/PhacoIOL; needed sedation despite generous topical
Despite maximal medical therapy and SLT laser, this patient was showing progressive glaucomatous damage with IOP readings in the mid 20's. Visual acuity prior to surgery was 6/60 OD and 6/15 OS with moderately shallow anterior chambers, pigmented debris covering angle, and synechiae inferiorly OS. Because of her dense cataracts, it was decided to combine her glaucoma surgery with cataract removal and lens implant.
Despite generous use of topical lidocaine jelly and sutenon's infusion of lidocaine & bupivicaine after the start of the surgery, this patient was not comfortable with me even touching her eye and required midazolam and fentanyl. Surgery proceeded well afterwards and her IOP was 3 with visual acuity of 6/30 uncorrected on the first post-operative day despite a fibrin reaction in the anterior chamber.
Case 3:
robschertzer #glaucoma #surgery 21Sep2009, 65 yo WM, prior TrabMMC, revised b/o leak, now Ahmed GV. Unusually straightforward dissection
This patient had a trabeculectomy in 1996 which I revised in 2005 because of painful hypotonous eye. He required a cataract extraction in 2007 and over a two year period began to need Cosopt and Alphagan to regain IOP control. With IOP ranging between 18-20 in this eye, he was starting to show progression of his glaucoma so we opted to implant an Ahmed Glaucoma Valve.
At the time of surgery, an unexpected finding was how easily his conjunctiva could be dissected from the underlying tissue. Usually in re-operations such as this, the conjunctiva is tightly adherent to the underlying tissue and requires extensive undermining of the tissue.
On the first post-operative day, his IOP was 6 with VA of 6/18.
23Sep2009
In addition to glaucoma surgery, I do perform cataract surgery in my glaucoma patients. Sometimes these pose interesting challenges which make them worth reviewing.
Case 4:
robschertzer #cataract #surgery #glaucoma patient 72 yo WM, PXF w/ prior TrabMMC, Malyugin Ring to enlarge pupil, trailing loop under iris
Case 5:
robschertzer #cataract #surgery #glaucoma patient 71 yo E Indian M, prior TrabMMC; refused IV line, moved eyes & strained but no complications.
Case 6:
robschertzer #cataract #surgery #glaucoma patient 46 yo Asian F, JOAG, s/p TrabMMC, hi myope soft nucleus, grooved then epinucleus setting rest, +3 IOL
Case 7:
robschertzer #cataract #surgery 66 yo WM, no #glaucoma- WOW. Easy divide/conquer 8 min skin-to-skin; nice break!
25Sep2009
Case 8:
robschertzer #glaucoma #surgery 74 yo soviet F, PXF prior failed TrabMMC & phaco; Ahmed GV after debriding
Prior to surgery, the IOP measured 36 on Pilo 2%, Xalatan, and Cosopt in her right eye. Although afraid to undergo further surgery as had Trabeculectomy in Jan 2008, required surgery as too high a risk of significant visual loss if did not proceed. On her Oct 1st visit, 1 week post-op, she is comfortable, relieved, and has an IOP of 4. The anterior chamber is very shallow with the tube on the iris and very close to the cornea. She has therefore been started on Atropine drops to help pull the iris back at the ciliary body level. The reason for the hypotony is most likely some leakage around the tube's insertion through the sclera.
Case 9:
robschertzer #glaucoma #surgery 76 yo WF, COAG, pseudophakic; heme w/in flap cauterized, still closed well
This bilaterally pseudophakic patient had also undergone SLT laser procedures in both eyes in the past. She was referred showing progression of her glaucoma despite this and the use of Travatan & Cosopt. Visual acuities were 6/12 and 6/9 with IOP readings of 23 and 16 @1445hrs. At the time of the trabeculectomy, there was some bleeding inside the scleral flap that required cauterization. This resulted in some blood in the subconjunctival space and some trickling into the anterior chamber at the conclusion of the surgery. Although seen later the same day following the surgery, as she was referred from out of town, she is being followed there for much of the post-operative period. She will be seen though by me at the 3 week mark in case a suture lysis is required.
Case 10:
robschertzer #glaucoma #surgery 81 yo WM, no prior surg., COAG OD, blind OS s/p CRVO. Trab MMC OD uncomplicated. No ung or shield as blind fellow eye
This patient had been referred because of uncontrolled elevated pressure in her only eye; she had lost her vision in the right eye following a Central Retinal Vein Occlusion (CRVO.) Pre-operatively on consultation, her IOP was 32 @1400hrs at which time low dose Diamox (125 mg po TID) was added to help tide her over until her surgery.
Her pressure was just 13 later the same day following her surgery. She lives far away so will be followed with her local ophthalmologist, even though I much prefer having patients see me for all their follow-up visits. I have a template in my Electronic Medical Record to help generate a customized letter back to the ophthalmologist who will be following my patients that includes mention of what procedure was performed, what the first post-op visit results were, and a detailed management plan for adjusting the medications over the subsequent two months. Although not a replacement for actually seeing the patient myself, this at least allows patients who otherwise would not have access to a tertiary care glaucoma specialist to get the surgery that they need.
Case 11:
robschertzer #glaucoma #surgery 91 yo WM!! Pre-op IOP 51 when stopped meds, progressing & 24 on meds, pseudophakic; Trab MMC only 1min MMM as thin
I really was not thrilled about having to operate on a 91 yo patient but the odds were just too high that he would go on to lose all of his vision if he did not have surgery. When seen in consultation the prior month, his IOP readings were 22 OD and 51 OS (!) @ 1435hrs. This patient had already undergone an SLT treatment and was on multiple glaucoma meds (DuoTrav Alphagan, and pilocarpine) and did have a pressure reading of 22 but he stopped taking the drops as he did not believe they were doing anything. Therefore, give the poor compliance, surgery was performed.
He returned on Oct 1 for his 1 week post-op visit with an IOP of just 8 and all looking good. Hopefully he will remain compliant to the prednisolone acetate drops for the remainder of his tapering course so that the surgery will not have been a waste.
Case 12:
robschertzer #glaucoma #surgery 73 yo WF, uveitic glauc, pseudophakic; Trab MMC creating tunnel entered AC, iridectomy then closed; all well.
This patient had an IOP of 68 when seen by her referring ophthalmologist in late August with severe uveitis. She had prior cataract surgery in this left eye and prior trabeculectomy in her fellow (right) eye. Visual acuity when I saw her initially in September was 6/15 OD and 6/12 OS with IOP readings of 22 OD and 42 OS @1145hrs taking DuoTrav, Cosopt, Alphagan, for her pressure and Maxidex dros and oral acyclovir for the inflammation. There was no evidence of intraocular inflammation. She was started on low dose Diamox (125 po TID) to tide her over until her surgery day.
At her one week post-op visit on October 1, her vision is 6/18 with an IOP of 6 and a low diffuse bleb. She is off to a good start.
Case 13:
robschertzer #glaucoma #surgery 78 yo WF, COAG, progressing w/ IOP 18, phakic, Trab MMC
When this patient was referred to me in mid August, her glaucoma was progressing despite IOP readings at 18 OU @ 0945hrs. Visual acuity was 6/18 OU, she had early cataracts OU, and was taking Xalatan and Combigan OU. She had undergone both ALT and SLT in each eye in the past. Optic nerve findings were quite striking for complete loss of the neuroretinal rim of her left eye and near total loss in the right. This, combined with thin corneas, helped explain why she was continuing to progress at 18mmHg pressure.
At her one week post-op visit on Oct 1, she gave a history of having been quite nauseated on the first post-op night. She was concerned that it could have been related to sedation at the time of her surgery but was, in fact, given almost nothing in the form of sedation or analgesia and had tolerated the surgery quite well with topical anaesthesia. In fact, given that her IOP at 1 week was 40 until her eye was gently massage to bring the IOP to 13, it was the high pressure that had made her sick on the first post-op day. This is a good reminder that patients should be warned that if they are nauseated following glaucoma surgery that there is a chance that their eye pressure is elevated and they should give us a call, even if after hours.